Serviços Personalizados
Artigo
Indicadores
Links relacionados
-
 Citado por Google
Citado por Google -
 Similares em Google
Similares em Google
Compartilhar
South African Dental Journal
versão On-line ISSN 0375-1562
versão impressa ISSN 0011-8516
S. Afr. dent. j. vol.71 no.4 Johannesburg Mai. 2016
RESEARCH
Incidence and predisposing factors for dry socket following extraction of permanent teeth at a regional hospital in Kwa-Zulu Natal
Vaneshree MudaliI; Ozayr MahomedII
IB. Dental Therapy (UKZN), PGDip Public Health (UKZN). Discipline of Public Health Medicine, University of Kwa-Zulu Natal, Durban
IIMBCHB (Natal), MBA, FCPHM (SA), M.Med-PHM (UKZN). Discipline of Public Health Medicine, University of Kwa-Zulu Natal, Durban
ABSTRACT
INTRODUCTION: Dry socket is one of the complications which may follow dental extractions. Whilst the exact pathogenesis is unknown, blood clot disintegration as a result of fibrinolysis remains the most acknowledged theory.
AIMS AND OBJECTIVES: To determine the incidence, distribution by tooth type and location and predisposing factors for dry socket in a public health facility.
METHODS: A retrospective review of the register and the records of patients who presented with dry socket at the facility were reviewed for the first quarter of 2015 (January-March). The following data were recorded: total number of patients their demographics, total number of permanent teeth extracted, number of dry sockets encountered and associated risk factors such as smoking, contraception and systemic illnesses.
RESULTS: 2214 patients were reviewed from whom a total of 2281 permanent teeth had been extracted. The overall incidence of dry socket was 1.8%, being more prevalent in females, in the second and third decades of life, and in mandibular teeth, more specifically in molars.
CONCLUSION: Dry socket occurrence is a painful but infrequent complication of tooth extraction and most commonly affects the mandibular sockets. Oral contraception and smoking independently or in combination with a traumatic extraction were the most prevalent predisposing factors.
INTRODUCTION
Dry socket, also known as alveolar osteitis, is a commonly encountered complication following dental extractions. The condition can be defined as: "postoperative pain in and around the extraction site, which increases in severity any time between one and three days after extraction, accompanied by a partially or totally disintegrated blood clot within the alveolar socket, with or without halitosis".1 The prevalence of dry socket has been reported to be as high as 35% in some cases.2 The most prominent characteristic of dry socket is debilitating pain, which responds poorly to narcotic and over-the-counter analgesics, generally leading to loss of productivity. It often requires a few postoperative visits to the dental practice to manage the pain, making it costly to both the patient and society.2
While the exact pathogenesis of dry socket is not entirely known, it is thought that dry socket occurs from increased fibrinolysis resulting in blood clot disintegration.3 The aetiology of dry socket is also not exactly understood but seems to be multifactorial - such factors include age, sex, use of oral contraceptives, smoking, extraction site, trauma from difficult extractions, poor oral hygiene, and vasoconstriction of local anaesthetics used.4,5
Various approaches have been advocated to decrease the occurrence of dry socket; including antibiotics, antibacterial mouthwashes, steroids, clotting agents, and medicaments. Chlorhexidine rinses and antibiotics appear to be the methods of choice. Despite the lack of understanding of the aetiology, the management of this painful condition nevertheless appears to be relatively simple and effective, involving cleaning and irrigating the affected socket followed by insertion of medicament such as Alvogyl whilst simultaneously reassuring the patient.6
Although dry socket is a relatively common oral health condition-affecting patients, there have been few studies conducted in South Africa that have looked specifically at prevalence and predisposing factors for the condition.
The aim of this study, therefore, was to determine the incidence and predisposing factors for dry socket cases in a public health facility that performs a high volume of extractions, as well as to describe the distribution of dry socket by tooth type and location.
METHODS
Study setting and design
This study was conducted at a regional public health facility with an outpatient dental headcount of approximately 14 000 patients per year. The study was a retrospective cross sectional study.
Study population
The study population included all patients who had undergone dental extractions of permanent teeth between the 1st of January and 31st March 2015.
Data sources and collection
The dental clinic register was used to identify the number of permanent teeth extracted, the number of dry socket cases encountered and the socio-demographic details (age and sex) of the participants in the study.
A retrospective review was conducted of the clinical records of all patients who had been diagnosed with dry socket following permanent teeth extraction. The following variables were recorded: type and location of the tooth/teeth extracted, reason for extraction(s) and relevant findings of the clinician who performed the extraction(s), social habits and medical history.
Data management and analysis
The collected data was entered into an electronic database and analysed descriptively.
Ethics
Anonymity of the patients was maintained as no identifiable information was recorded. The study obtained ethical approval from the Bio-Medical Research and Ethics Committee (BREC) at the University of Kwa-Zulu Natal (BE 252/15). Permission to conduct this study was also obtained from the facility as well as from the Provincial Department of Health.
RESULTS
A total of 2214 patients had attended the dental clinic for tooth extraction between the 1st of January and 31st of March 2015, and a total of 2281 permanent teeth had been extracted. Sixty percent (1204) of patients were between the ages of 21 and 40, whilst 18% (402) were less than 20 years old. A total of 42 extractions were complicated by dry socket in the first quarter of 2015 resulting in an incidence of 1,84 dry sockets per 100 extractions with a 2:1 female predominance (Table 1). Seventy percent (29/42) of the dry sockets occurred in patients between the ages of 21 and 40 years.
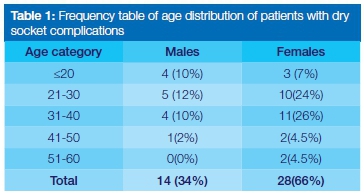
Distribution of dry socket by tooth type
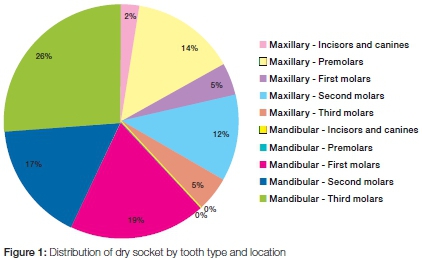
Dry sockets occurred most frequently in the mandibular arch (62%). In terms of individual teeth, mandibular third molars accounted for the highest percentage of affected sockets (26%) followed by mandibular first molars (19%) and mandibular second molars (17%) (Figure 1).
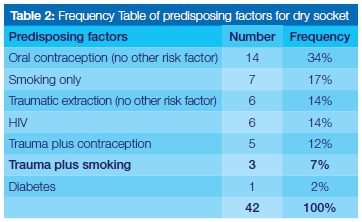
Risk factors for dry socket
Nineteen of the twenty eight females (67%)who developed dry socket were on some sort of oral contraception, with this being the only predisposing factor for 14 (50%) of the group. Smoking was the most common predisposing factor in males with 72% (10/14) of those who developed dry socket having a history of smoking. Traumatic extractions was the only factor in six (14%) of the cases, but when in combination with oral contraception and smoking was identified in 34% (14) of the cases. Six (14%) of the patients with dry socket were HIV positive, whilst one patient had diabetes mellitus.
DISCUSSION
Dry socket is a painful condition that may occur after a dental extraction and is often distressing to the patient. Although the exact pathogenesis of dry socket is not fully understood, it is thought to occur from increased fibrinolytic activity resulting in blood clot disintegration.7 In this study, the incidence of dry socket was 1,8%, which is slightly higher than the findings of a Nigerian study that showed an incidence of 1,4%.8 However, the findings presented are consistent with other studies that show an incidence of between 1% and 4%.9 The variability in the incidence of dry socket could possibly be attributed to the different assessment methods and the variations in diagnostic criteria.
The incidence of dry socket was highest in the third and fourth decades of life, in strong agreement with other studies.8 Why this should be is still not known but it has been postulated that the presence of well-developed alveolar bone and the relative infrequency of periodontal diseases in this age group make tooth extraction more difficult. Seven patients in this study were below 20 years of age, contrary to the perception that dry socket does not occur below 18 years of age.8
A female predominance (2:1) was noted. This finding is similar to a study conducted in Palestine which confirmed a higher incidence of dry socket in females.10 Two reasons have been suggested to explain the female predominance; namely, better health-seeking behaviour of females11 and the use of oral contraceptive pills12 which increase fibrinolytic activity in blood and saliva during the menstrual phase, affecting the stability of the blood clot. In the current study, 71.4% of females who developed dry socket were using oral contraceptives.
Regarding anatomical site, mandibular teeth, more specifically molars, were more affected than maxillary teeth, consistent with a study conducted in Sri Lanka.13 In addition, dry socket was more common in mandibular third molars, followed by mandibular first molars and mandibular second molars; consistent with the findings of other studies.9 The specificity of these sites may be related to the decreased vascularity, greater bone density and a diminished capacity in forming granulation tissue.13 It has also been suggested that difficulty of traumatic extractions may be a cause.1 It is thought that trauma results in compression of the alveolar bone, reduction in blood perfusion and thrombosis of underlying blood vessels leading to increased fibrinolytic activity.1
Numerous studies have demonstrated the link between dry socket and smoking, with some studies pointing towards a dose dependent relationship.2 The risk of developing dry socket is reported to be significantly greater in smokers than non-smokers.14 It was found that 31% of the patients in the current study that developed dry socket were smokers, all of whom were male. Although smoking has been associated with an increased incidence of dry socket, it is unclear of the exact causal mechanism. It is possible that the increased risk associated with smoking is related to substances in tobacco and its smoke, particularly nicotine, cotinine, carbon monoxide, and hydrogen cyanide which are cytotoxic to the cells involved in wound healing.15 Nicotine increases platelet adhesiveness, raising the risk of microvascular occlusion, and tissue ischemia.16 It has also been postulated that smoking is associated with the release of catecholamines, resulting in vasoconstriction and decreased tissue perfusion.16 Other authors have suggested that the heat from the burning tobacco, along with its byproducts, could contaminate the surgical site. This, together with the suction applied to the cigarette could dislodge the clot from the alveolus and interrupt healing.17
In this study, seven patients who developed dry socket had underlying medical conditions; however, current opinion reflected in the literature indicates that systemic conditions do not play a role in the occurrence of dry socket.2
All extractions performed during this study were under local anaesthetic containing a vasoconstrictor. Other studies indicate that the resulting local ischemia has no implication in the pathogenesis of dry socket.2 Further, dry sockets have been known to occur in patients who underwent general anaesthesia for the extractions.
Study limitations
This study was conducted in a single regional hospital and was dependent on the accuracy and completeness of the clinical records. Therefore, detailed information regarding the duration of a smoking habit and the quantity of cigarettes smoked, the use of oral contraceptives, oral hygiene status and the degree of difficulty in extractions were not adequately recorded for all patients. The study was a descriptive cross sectional study and did not allow for detailed statistical analysis to determine associations.
CONCLUSION
Dry socket occurrence is a painful but infrequent complication of tooth extraction and most commonly affects the mandibular teeth. Oral contraception and smoking independently or in combination with a traumatic extraction were the most prevalent predisposing factors for dry socket in our study.
It is important that these underlying predisposing factors (smoking and oral contraceptive use) are recognized and that patients are appropriately counselled.
References
1. Blum, I. Contemporary views of dry socket (alveolar osteitis): a clinical appraisal of standardization, aetiopathogenesis and management: a clinical review. International Journal of Oral Maxillofacial Surgery, 2002;1:309-17. [ Links ]
2. Nusair, Y, Younis, M. Prevalence, clinical picture, and risk factors of dry socket in a Jordanian dental teaching centre. Journal of Contemporary Dental Practice, 2007;3(8):53-63. [ Links ]
3. Upadhyaya, C, Humagain, M. Prevalence of dry socket following extraction of permanent teeth at Kathmandu University Teaching Hospital (KUTH), Dhulikhel, Kavre, Nepal: A study. Kathmandu University Medical Journal, 2010;8(29):18-24. [ Links ]
4. Akinbami, B, Godspower, T. Dry Socket: incidence, clinical features, and predisposing factors. International Journal of Dentistry, 2014 June 2.doi 1155/2014/796102. [ Links ]
5. Claesson, L., Lundberg, I. (n.d.). Dry socket-prevalence and risk factors in a Pakistani population. Odontologiska Institutionen, Karolinska Institutet. [ Links ]
6. Veale, B. Alveolar osteitis: a critical review of the aetiology and management. Oral Surgery, 2015;8(2):68-77. [ Links ]
7. Birn, H. Etiology and pathogenesis of fibrinolytic alveolitis ('dry socket'). International Journal of Oral Surgery, 1973;2(5):211-63. [ Links ]
8. Oginni, F, Fatusi, F, Alagbe, F. A clinical evaluation of dry socket in a Nigerian teaching hospital. Journal of Oral and Maxillofacial Surgery, 2003;61(8):871-6. [ Links ]
9. Jaffar, N, Nor, G. The prevalence of post-extraction complications in an outpatient dental clinic in Kuala Lampur Malaysia - a retrospective survey. Singapore Dental Journal, 2000;23(11):24-8. [ Links ]
10. Younis, M, Hantash, R. Dry Socket: frequency, clinical picture, and risk factors in a Palestinian Dental Teaching Center. The Open Dentistry Journal, 2011; 5:7-12. [ Links ]
11. Preshaw, P, Fisher, S. Routine review of patients after extraction of third molar: Is it justified? British Journal of Oral and Maxillofacial Surgery, 1997;35:339-46. [ Links ]
12. Hermesch, C., Hilton, T, Biesbrock, A, Baker, R, Cain-Hamlin, J, McClanahan, S, Gerlach, R. Perioperative use of 0.12% chlorhexidine gluconate for the prevention of alveolar osteitis: efficacy and risk factor analysis. Oral Surgery, Oral Medicine, Oral Pathology, Oral Radiology, and Endodontics, 1998;85(4):381-7. [ Links ]
13. Amaratunga, N, CM, S.. A clinical study of dry socket in Sri Lanka. British Journal of Oral Maxillofacial Surgery, 1998;26(5):410-8. [ Links ]
14. Meechan, J, Macgregor, I, Rogers, S, Hobson, R, Bate, J, Dennison, M. The effect of smoking on immediate post-extraction socket filling with blood and on the incidence of painful socket. British J ournal of Oral Maxillofacial Surgery, 1988;26:402-9. [ Links ]
15. Al-Belasy, F. The relationship of "shisha" (water pipe) smoking to postextraction dry socket. Journal of Oral Maxillofacial Surgery, 2004;62:10-4. [ Links ]
16. Cryer, P, Haymond, M, Santiago, J, SD, S. Norepinephrine and epinephrine release and adrenergic mediation of smoking-associated hemodynamic and metabolic events. New England Journal of Medicine, 1976;295:573-7. [ Links ]
17. Sweet, J, Butler, D. The relationship of smoking to localized osteitis. Journal of Oral Surgery, 1979;37:732-5. [ Links ]
 Correspondence:
Correspondence:
Ozayr Mahomed
Discipline of Public Health Medicine
University of Kwa-Zulu Natal
Durban, 4001
Tel: 031 260 4382
Fax: 086 666 6601
E-mail: mahomedo@ukzn.ac.za













