Services on Demand
Article
Indicators
Related links
-
 Cited by Google
Cited by Google -
 Similars in Google
Similars in Google
Share
South African Dental Journal
On-line version ISSN 0375-1562
Print version ISSN 0011-8516
S. Afr. dent. j. vol.70 n.9 Johannesburg Oct. 2015
RESEARCH
An investigation into the incidence and distribution of fractures of the coronoid process in patients presenting at the Sefako Makgatho Health Sciences University, Oral Health Centre
AS SinghI; MMR BouckaertII; JM MchengaIII; CJ PerumalIV
IBDS, MSc, MDS, MDent. Head of Department of Maxillofacial and Oral Surgery, Greys Hospital
IIBChD, MDent. Department of Maxillofacial and Oral Surgery, Sefako Makgatho Health Sciences University
IIIBEd, BDS, PDD, MDent. Department of Maxillofacial and Oral Surgery; Sefako Makgatho Health Sciences University
IVBDS. Department of Maxillofacial and Oral Surgery. Greys Hospital
ABSTRACT
Isolated coronoid fractures, especially those that are due to direct trauma are very uncommon because the coronoid process is anatomically sheltered by the zygomatic complex, and the associated muscles. Further, such fractures can easily be missed. The causes of coronoid fractures include road traffic accidents, interpersonal violence, gunshot injuries, third molar extractions, pathology and bilateral sagittal split osteotomies.
The aim of this study was to assess the incidence and distribution of coronoid fractures among trauma patients who had presented to the Maxillofacial and Oral Surgery Department, Sefako Makgatho Health Sciences University, between the years 2005 to 2008. One thousand seven hundred and fifty five patients who reported to the Oral and Dental Hospital had sustained facial bone fractures, of which one thousand two hundred and twenty two had suffered mandibular fractures. Fifteen (1.23%) of these patients were found to have a fracture of the coronoid process. The main causes of injury were seen to have been gunshots and assault, with the latter having been the major contributor. All the coronoid fractures were treated conservatively.
INTRODUCTION
The mandible is a horse-shoe shaped bone with various anatomical features such as the coronoid process, condyle, ramus, angle, body, symphysis and alveolus occurring bilaterally. The coronoid process is located anterior to the condyle and superior to the mandibular notch. It provides attachment to the temporalis muscle. The weakest sites are believed to be the third molar, the canine teeth and the condyle areas. The arterial supply of the mandible is derived from the external carotid artery through the maxillary artery, a branch of which forms the inferior alveolar artery that passes through the mandibular canal and exits through the mental foramen as the mental artery.
Fractures of the coronoid processes are uncommon1 because the structure is anatomically sheltered by the zygomatic complex, and the associated muscles. Clarkson and co-workers2 first reported coronoid fractures among British troops during World War II. The etiological factors of coronoid fractures include road traffic accidents, interpersonal violence, gunshot injuries, third molar extractions, pathology and bilateral sagittal split osteotomies.
Fractures of the mandible are classified based on the type and the anatomical site. The types of fractures may be classified as either greenstick, simple, comminuted, compound, displaced or undisplaced and pathological. Anatomical sites of the fractures may be classified as dentoalveolar, condylar, coronoid, ramus, angle, body, parasymphysis and symphysis fractures. Shen and co-workers classified coronoid fractures as: fracture of the coronoid base; of the upper coronoid process; comminuted fractures of the coronoid process and those affecting both the coronoid process and the mandibular ramus.3
When evaluating mandibular fractures, it is necessary to obtain a clinical history and to perform a physical examination.4 Fractures should be suspected in severe case of trauma, especially when there has been high impact. A blow from a fist often results in a single, non-displaced fracture. Motor vehicle accidents are usually associated with multiple fractures which are often comminuted. A blow to the chin may result in bilateral condylar fractures. An angled blow inflicted laterally to the parasymphysis area may cause contralateral condylar or angle fractures. The different types of displacements of fractured segments are often determined by factors such as the direction and degree of force, the integrity of the periostium, the extent of interdigitation of the fractured ends, the direction of the fracture lines and the pull of the muscles which insert on the mandible. Patients with coronoid fractures usually present with pain and limited mouth opening. Treatment is dependent on the amount of displacement present together with clinical signs and symptoms. Severely displaced fractures often are treated surgically by open reduction, whereas undisplaced fractures are usually treated conservatively or by closed reduction. Untreated coronoid fractures may result in adhesions of the fracture segment to the surrounding tissues resulting in fibrous ankylosis.
The current retrospective study of coronoid process fractures is the first to be conducted at the Department of Maxillofacial and Oral Surgery, Sefako Makgatho Health Sciences University.
LITERATURE REVIEW
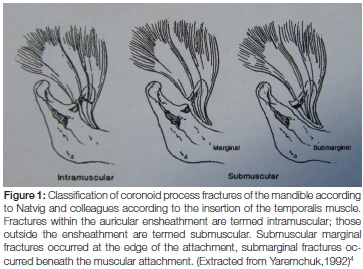
Several factors contribute to fractures of the coronoid process. Most are due to direct blunt or penetrating trau-ma.1 Iatrogenic causes such as extractions of maxillary and mandibular third molars, cystectomies and sagittal split ramus osteotomies can contribute. Coronoid fractures have been divided anatomically into intramuscular and submuscular fractures. (Figure 1.)
A retrospective study in Baghdad reported an increase in the numbers of patients presenting with mandibular fractures.5 The study also showed a male predominance, a result similar to that reported in other studies. The pattern of etiology in Baghdad was found to have been assault and falls from a height, which over the last 10 years has changed to bullet and shell injuries. During the period 1995 to 1996 there were two coronoid fractures recorded among 150 mandibular fractures. This however, has changed. Data gathered over the period 2005 to 2006 recorded one coronoid fracture among 100 mandibular fractures. Trends in the treatment of mandibular fractures were analysed over a five-year period, 2007 to 2011,6-7 the study including 335 patients who had sustained 406 mandibular fractures. There was a higher incidence among males with a male: female ratio of 2.8:1. The age range was 1-72 years with a mean age of 28.5 years. The most commonly fractured site was the condyle (36.2%) and the least common was the coronoid process (0.5%.) The majority (92.5%) of the patients were treated by open reduction.
A 2% deformity in bone is sufficient to trigger a fracture process. Boole and co-workers (2001) reported a 1% incidence of coronoid fractures among 5196 patients.8 In a study conducted in India, 2103 mandibular fractures occurred amongst a total of 2901 facial bone injuries.9 Road traffic accidents were the major contributing factor to mandibular fractures. Three percent occurred in the ramus of the mandible while the least frequent fracture affected the coronoid processes (2%). Closed reduction (78%) was the preferred form of treatment modality for the management of the fractures.9
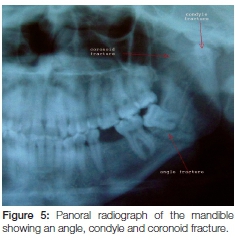
A five-year study of 237 patients in Iran over the period 1996 to 2001 revealed 173 mandibular fractures.10 The majority occurred in the condylar region while 29.3% were located in the symphyseal and parasymphyseal regions. Least frequently, the coronoid processes were found in only 1.2% of the 173 fractures.10 In another study, fifty two cases were reported with coronoid process fractures, which constituted 2.9% of all facial fractures evaluated.11 Twelve were isolated coronoid fractures (23%) while the remainder of the 40 cases were associated with other maxillofacial injuries. (Figures 2, 3, 4 and 5)
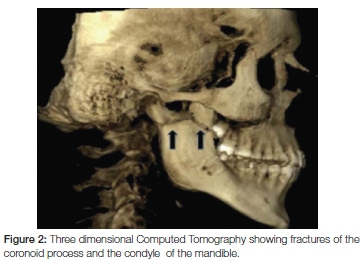
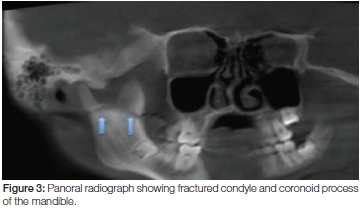
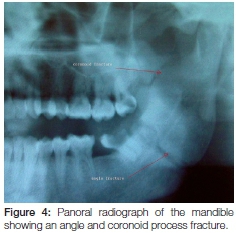
While road traffic accidents remain the main cause of mandibular fractures, a case reported in Japan revealed that the probable cause of coronoid fractures in that instance to have been an acute reflex contraction of the temporalis muscle.12 This break was associated with a subcondylar fracture which occurred indirectly. Another case of bilateral reflex muscular contraction causing fracture of the coronoid process was reported in Wales.13 These fractures had occurred after a blow to the left temporal region after an assault. There was no evidence of direct trauma to the facial bones, hence, the probable cause of an acute reflex contraction of the temporalis muscles is plausible.
An aneurysmal bone cyst occurring in the left coronoid process was seen in a 17-year-old male patient in India.14 The cyst was surgically removed via a superior approach to the temporal fossa via a pre-auricular incision. The procedure required the fracturing of the left coronoid process. Whilst this may be regarded as an iatrogenic fracture, if the lesion was not removed, the coronoid process would have remained prone to fracture.
TREATMENT
Treatment options for mandibular coronoid fractures range from no treatment in isolated non-displaced fractures of the coronoid process to open reduction in cases of severe displacement. Reduction is essential when the fracture fragment impinges on the zygomatic bone, resulting in trismus.15 An unusual fracture occurred in Boston in a seizure-prone patient.3 There was an oblique submuscular displaced fracture running from the depth of the mandibu-lar notch to a point immediately behind the distal end of the alveolar process. Treatment required reduction and internal fixation, using plates and screws, hence avoiding intermaxillary fixation in that susceptible patient.3 All the coronoid fractures in this study were treated conservatively.
MATERIALS AND METHOD
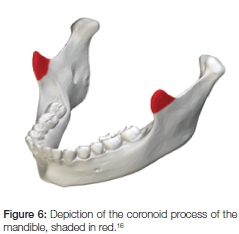
For the purpose of this study, the coronoid process was defined as the triangular antero-superior extension of the ramus of the mandible as depicted in Figure 6.
Radiographic and clinical data spanning a three year period (1 January 2005 to 31 December 2008) were obtained from the files of patients in the Department of Maxillofacial and Oral Surgery, Sefako Makgatho Health Sciences University
The records of 4000 patients who had presented with trauma-related maxillofacial injuries were retrieved from the clinic archives. The cause, nature of injury and patient demographics such as gender, age and date of injury of those patients who had a fracture of the coronoid process were recorded in a data collection sheet and analysed in Microsoft® Excel.
RESULTS
One thousand seven hundred and fifty five patients had sustained facial fractures. One thousand two hundred and twenty two patients had suffered mandibular fractures. Fifteen (1.23%) of these patients had undergone a fracture of the coronoid process.
Age
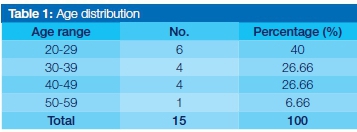
The age distribution is demonstrated in Table 1. The mean age was found to have been 33.6 years.
Gender
All 15 patients were males.
Cause of injury
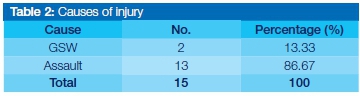
There were two causes of injury, gun shot wounds (GSW) and assault, the latter having been the major contributor. Table 2 summarises the cause of injury.
Site of injury
There was no obvious side predilection. (Table 3).
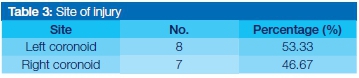
The frequency of isolated coronoid fractures and in association with other facial fractures.
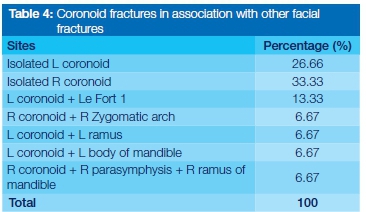
Table 4 presents data showing how coronoid fractures occurred alone or in combination with other mandibular fractures.
DISCUSSION
The prevalence and incidence of coronoid fractures varies only slightly in geographic distribution. In Brazil, a 1% incidence of coronoid fractures among 5196 patients was reported whereas in India a 2% incidence among 2103 patients was reported and in Greece a 2.9% incidence was reported.1,9,11 This study found a 1.23% incidence of coronoid fractures among 1222 patients who had sustained mandibular fractures. This equated to a 0.84% incidence among the 1755 patients who sustained facial fractures.
The cause of injury varies in different regions. In Japan, road traffic accidents were the major contributing factor to coronoid fractures.12 Coronoid injuries are not only related to trauma, however but also may be due to acute reflex contraction of the temporalis muscle.13 Pathology in the region of the coronoid process has also been cited as a causal factor in such fractures.14 In Bhagdad the trend in etiology changed from assaults and falls from heights to bullets and shell injuries.7 This South African study found gunshot injuries (13.3%) and assaults (86.7%) to have been the two contributing factors. None of the patients sustained a coronoid fracture due to acute reflex contraction of the temporalis muscle, or to pathology.
The literature does not report extensively on age or gender in relation to the occurrence of coronoid fractures. Only males were affected in the current study. This study found an age distribution of 20 to 59 years with a mean age of 33.6 years. The majority of the injuries occurred in the 20 to 29 year age group. Although in this study there was little difference in the side affected (47% to 53%), any tendency, it may be speculated, could be due to the left or right handedness of the assailant in the case of assault.
Most coronoid fractures of the mandible occur in combination with other facial injuries. A 1985 literature search project revealed 52 reported cases of coronoid process fractures, which constituted 2.9% of all mandibular fractures."Twelve were isolated coronoid fractures (23%) while the remaining 40 cases occurred in association with other maxillofacial injuries. Another study reported that the propensity of coronoid fractures occurring in the presence of pathology in the mandible may be increasing.14
In the current study 60% of the cases presented as isolated coronoid fractures, while 40% were in association with fractures at other sites in the mandible and facial bones. The highest number of coronoid fractures (13.33%) was associated with Le Forte I fractures. The treatment for these fractures varies depending on the severity of the fracture. Yaremchuk (1992) treated the fractures with open reduction and internal fixation.3 All fractures in the current study were treated by conservative means. No long-term follow up reviews of these patients were carried out, but the records showed that within the time limits of the study, no patients returned with any fracture-related problems.
CONCLUSION
It is evident from the results of this study that mandibular coronoid fractures are rare. The aetiology varies from pathology to trauma. Males are affected more than females, as males are generally more exposed to violent insults. Although coronoid fractures are the least reported among mandibular fractures, they deserve attention. Treatment methods remain controversial. The general consensus is to treat coronoid fractures conservatively. However, there are no studies to date which compare the efficacies of different treatment modalities, nor the long term effects of such treatments.
Although not much attention seems to be given to man-dibular coronoid fractures, the pain and discomfort and long term outcomes, such as trismus and ankylosis, make the issue worthy of discussion and attention.
ACRONYM
GSW: gun shot wounds
References
1. Oliveira DM, Vasconcellos RJH, Filho JRL, Cypriano RV. Fracture of the coronoid and pterygoid processes by firearms: case report. Brazilian Dental Journal. 2007; 18: 168-70. [ Links ]
2. Clarkson P, Wilson TH, Lawrie RS. Treatment of 1000 jaw fractures. British Dental Journal. 1946; 80: 107. [ Links ]
3. Shen L, Li J, Li P, Long J, Tian W, Tang W. Mandibular coronoid fractures: Treatment options. International Journal of Oral & Maxillofacial Surgery, 2013; 4: 1-6. [ Links ]
4. Yaremchuk M.J., Rigid internal fixation of a displaced mandibular coronoid fracture. Journal of Craniofacial Surgery. 1992; 3: 226-9. [ Links ]
5. Mahdi AGM & Ali IAA. A retrospective analytic study of mandibular fracture patterns in two different periods in Bhagdad. Journal of Oral and Maxillofacial Surgery, Medicine and Pathology, 2012; http://dx.doi.org/10.1016/j.ajoms.2012.08.006. [ Links ]
6. Ongodia D, Li Z, Zhou HH, Li Z.B. Comparative analysis of trends in the treatment of mandibular fractures. Journal of Oral and Maxillofacial Surgery, Medicine and Pathology. 2013; http://dx.doi.org/10.1016/j.ajoms.2013.01.005. [ Links ]
7. Ahmed N, Katherine G. How to manage fractures of the mandible - a simple guide. Face Mouth and Jaw Surgery: International Trainee Journal of Oral & Maxillofacial Surgery. 2012; 2: 12-21. [ Links ]
8. Boole JR, Holtel M, Amoroso P, Yore M. 5196 mandible fractures among 4381 active duty army soldiers, 1980 to 1998. Laryngoscope. 2001; 111: 1691-6. [ Links ]
9. Rai B, Dhattarwal S, Jain R, Kangra V, Bhardawaj D.N. Road traffic accidents: site of fracture of the mandible. The Internet Journal of Epidemiology. 2007; 4: 1-4. [ Links ]
10. Motamedi MHK. An assessment of maxillofacial fractures: A 5 year study of 237 patients. Journal of Oral and Maxillofacial Surgery. 2003; 61: 61-4. [ Links ]
11. Rapidis AD, Papavassiliou D, Papadimitriou J, Koundouris J, Zachariadis N. Fractures of the coronoid process of the mandible. An analysis of 52 cases. International Journal of Oral Surgery. 1985; 14: 126-30. [ Links ]
12. Shinya Y, Noritaka O, Kazuhiro O, Yuri I. Fractures of the condylar and coronoid processes of the mandible: A case report. Hospital, Dental and Oral -Maxillofacial Surgery. 2006; 18:m 101-3. [ Links ]
13. Philip M, Sivarajasingam V, Shepherd J. Bilateral reflex fracture of the coronoid process of the mandible. A case report. International Journal of Oral and Maxillofacial Surgery. 1999; 28: 195-6. [ Links ]
14. Goyal A, Tyagi I, Syal R, Agrawal T, Jain M. Primary aneurysmal bone cyst of coronoid process. Biomed Central Ear, Nose and Throat Disorders. 2006; 6: 1472-7. [ Links ]
15. Stierman Kl, Bailey BJ, Quinn F.B. Mandibular fractures. http://www.utmb.edu/otoref/grnds/Mandible-fx-0006.htm. Accessed 10/06/2013. [ Links ]
16. https://www.google.co.za/search?q=PICTURE+OF+CORONOID+PROCESS+OF+
17. MANDIBLE&biw=1366&bih=667&tbm=isch&imgil=. Accessed 10/06/2015.
 Correspondence:
Correspondence:
As Singh
Head of Department of Maxillofacial and Oral Surgery, Greys Hospital
Tel: 033 897 3164
E-mail: avin.singh@kznhealth.gov.za













