Services on Demand
Article
Indicators
Related links
-
 Cited by Google
Cited by Google -
 Similars in Google
Similars in Google
Share
South African Dental Journal
On-line version ISSN 0375-1562
Print version ISSN 0011-8516
S. Afr. dent. j. vol.70 n.4 Johannesburg May. 2015
RADIOLOGY CASE
Maxillo-facial radiology case 131
A UysI; Z YakoobII
IBSc, BChD, Dip. Odont(Materials), Dip. Odont.(Endo), MSc(Odont.). Department of Oral Pathology and Oral Biology, School of dentistry, University of Pretoria, e-mail: andre.uys@up.ac.za
IIBChD, PDD, MSc (Maxillofacial Radiology). Department of Oral Pathology and Oral Biology, School of Dentistry, University of Pretoria, e-mail: zarah.yakoob@up.ac.za
INTERPRETATION
The radiographic images display the different radiographic features that may be found in osteosarcoma of the jaws. Osteosarcoma is a malignant neoplasm of bone that is rare in the jaws compared to the incidence in long bones. The malignant osteoblasts found in osteosarcoma produce osteoid.1 These lesions occur in all racial groups, and occur most often in the third and fourth decades. The most common symptoms are swelling, pain, tooth mobility, paraesthesia and nasal obstruction. The radiographic features of osteosarcoma may vary. Localised widening of the periodontal ligament spaces and loss of lamina dura is in most cases the earliest sign. As the tumour progresses it may produce an osteolytic, osteoblastic or mixed pattern. The production of reactive bone to form sunray appearance is seen in only 25% of cases.2 The imaging tool which most accurately demonstrates the degree of bone involvement is CT.3
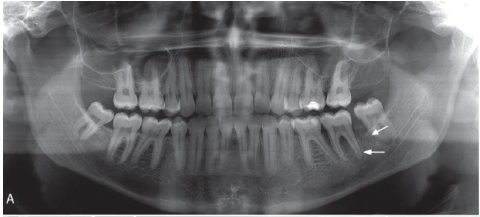
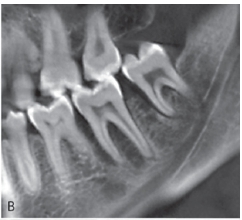
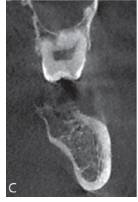
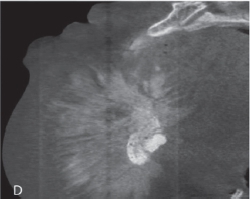
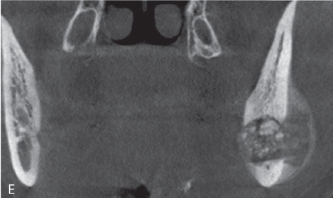
Fig. 1A is a panoramic radiograph of a 27 year old male. An osteosarcoma is present in the body of the left mandible in the area of tooth 37 and 38. Note the widened periodontal ligament spaces (arrows), loss of lamina dura and the loss of bone around tooth 37 and 38 resulting in an osteolytic pattern. Fig. 1B and 1C is a reconstructed panoramic CBCT view and coronal view respectively from the same patient seen in 1A. The widened periodontal ligament space can clearly be observed at the mesial root of tooth 38. A change in the trabecular bone pattern mesial of the 37 and in the interradicular area between the roots of the 37 is also seen. The coronal slice in figure 1C demonstrates the loss of cortical bone in the superior aspect of the mandible and the change of the trabecular bone pattern. Fig. 1D is a sagittal CBCT view of the symphysis area of the mandible of a 44 year old female with an osteosarcoma. Destruction of cortical bone with a periosteal reaction at the periphery forming a sunray or speculated periosteal reaction is present. Fig. 1E is a coronal view of the left mandibular ramus of a 23-year-old female patient with an osteosarcoma. The internal structure of the lesion has a mixed radiolucent-radiopaque appearance. The normal osseous architecture within the lesion is destroyed and buccal expansion is present.
Lesions that may present with similar radiographic features include osteomyelitis, metastases, chondrosarcoma, and Ewing sarcoma. These lesions should be included in differential diagnoses. In those cases where the only radiographic sign is localised widening of the periodontal ligament, the differential diagnoses should include traumatic occlusion and periapical pathology. It is due to these early signs that the oral health professional can make an early diagnosis, which should result in a better prognosis.
References
1. Nakayama E, Sugiura K, Ishibashi H, Oobu K, Kobayashi I, Yoshiura K. The clinical and diagnostic imaging findings of osteosarcoma of the jaw. Dentomaxillofac Radiol 2005; 34: 182-8. [ Links ]
2. Samraj L, Kaliamoorthy S, Venkatapathy R, Oza N. Osteosarcoma of the mandible: A case report with an early radiographic manifestation. Imaging Sci Dent 2014; 44: 85-8. [ Links ]
3. Wang S, Shi H, Yu Q. Osteosarcoma of the jaws: demographic and CT imaging features. Dentomaxillofac Radiol 2012; 41: 37-42. [ Links ]













