Services on Demand
Article
Indicators
Related links
-
 Cited by Google
Cited by Google -
 Similars in Google
Similars in Google
Share
South African Dental Journal
On-line version ISSN 0375-1562
Print version ISSN 0011-8516
S. Afr. dent. j. vol.69 n.9 Johannesburg Oct. 2014
CASE REPORT
Plunging ranula: an unusual multilocular presentation
M MabongoI; B BuchII; S P NgwenyaIII
IBDS (Wits); MChD (UCT); Head: Clinical Unit, Department of Maxillo-Facial and Oral Surgery, School of Oral Health Sciences, University of the Witwatersrand, Johannesburg
IIBSc (Hons)(Natal); SED (UCT); BDS (Wits); MSc (Dent)(Wits); Emeritus Professor-University of Pretoria, Part-time consultant-Division of MFO Radiology, Department of General Dental Practice, School of Oral Health Sciences, University of the Witwatersrand, Johannesburg
IIIBDS; MDent (Medunsa); Head: Department of Oral Pathology, School of Oral Health Sciences, University of the Witwatersrand, Johannesburg
SUMMARY
A 32 year-old male patient who was HIV positive presented at the Wits Oral Health Centre complaining of a large swelling of the left submandibular region of three years' duration. The swelling was non-tender, soft and doughy on palpation and appeared to be crossing the midline. Bilateral sub-mandibular and submental lymphadenopathy was present. Intraorally the lesion caused considerable elevation of the floor of the mouth and impaired the flow of saliva. Fluid from the lesion was aspirated and the patient sent for MRI examination. These images revealed a multilocular cystic lesion causing disruption of the mylohyoid muscle. The aspirate consisted of a thick, bloody fluid which tested positive for salivary amylase. A provisional diagnosis of plunging ranula was made. The multilocular nature of the lesion seen on MRI prompted a more extensive surgical approach in order to prevent recurrence. Consequently the sublingual gland was removed via an intraoral approach while the multilocular cyst was dissected by means of a submandibular approach in order to effect complete removal. Microscopic examination of the submitted specimen confirmed the clinical diagnosis of a plunging ranula.
CASE REPORT
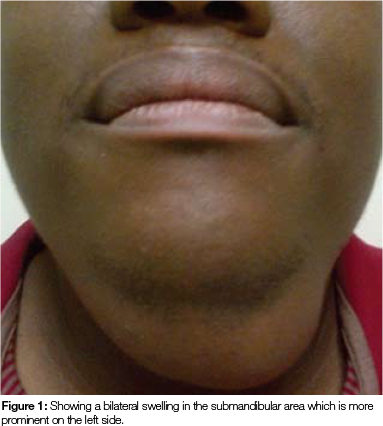
A 32 year old male patient presented at the Wits Oral Health Centre complaining of a large swelling of the submandibular area which he reported to have been of three years' duration, and which seemed to be actively enlarging. Clinical examination revealed a swelling in the submandibular area that presented as a bilateral mass. The swelling was non-tender and felt soft and doughy on palpation. The borders of the lesion appeared poorly defined and bilateral submandibular and submental lymphadenopathy was present. The overlying skin was normal in colour and texture and the inferior borders of the mandible could be palpated on both sides. Intraoral examination revealed a swelling which had produced considerable raising of the floor of the mouth on the left side. The salivary flow from the submandibular duct on the left side was notably less as compared with that on the right.
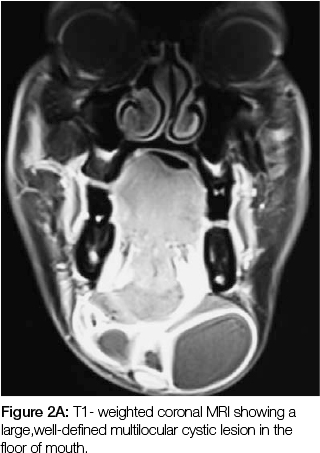
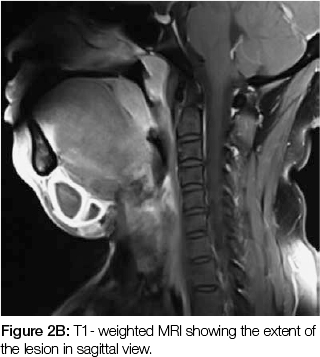
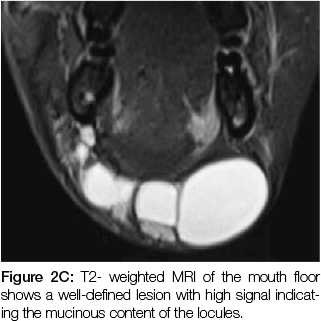
Aspiration of the fluid from the lesion was carried out and the patient sent for magnetic resonance imaging (MRI), which revealed a multilocular cystic lesion causing disruption of the mylohyoid muscle. Communication between the lesion and the floor of the mouth was noted.The lesion consisted of a number of cystic spaces separated by remarkably thick walls, the largest locule measuring 8x3cm. The contents of the locules appeared dark on T1- weighted images and bright on T2, indicating the presence of mucin. The presentation was suggestive of a plunging ranula but other differentials included a dermoid cyst, a cystic hygroma, a branchial cyst and a thyroglossal cyst.
A thick bloody fluid was aspirated from the lesion. The aspirate was tested for salivary amylase, and proved positive. This is suggestive of a saliva-containing cyst, and hence a provisional diagnosis of a plunging ranula was made, In accordance with the appearance on the MRI scan.
The lesion, together with the left sublingual gland, was surgically removed in theatre. Both intraoral and extraoral approaches were used. The sublingual gland was removed via an intraoral approach. Intraoperatively a direct communication between the left sublingual gland and the cyst was identified and ligated after which the gland was removed. A submandibular incision was made and the cyst removed together with the ligature. The specimen was subsequently delivered to the laboratory for a histopathological diagnosis.
Microscopic examination of the submitted specimen reveals a cystic space lined by fibrous connective tissue with a mixed inflammatory infiltrate comprising vacuolated macrophages, lymphocytes, neutrophils and eosinophils. The associated mucinous glands show a largely chronic inflammatory infiltrate and dilated ducts. The microscopic features are those of a mucous extravasation cyst and are consistent with the clinical impression of a ranula.
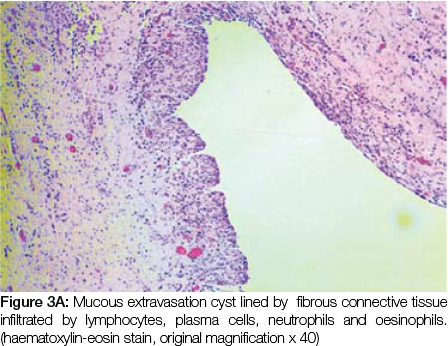
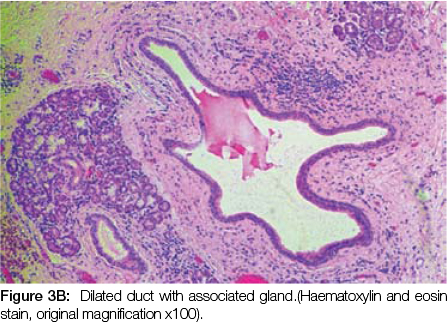
DISCUSSION
A ranula is a mucocoele which occurs in the floor of the mouth and is not an uncommon lesion. It is caused by spillage of mucin, usually from injury to the sublingual gland or to a minor salivary gland in the floor of the mouth. If, however, the mucus tracks through the mylohyoid muscle and produces swelling in the neck, the result is a plunging ranula.1 Such a condition requires more extensive treatment. A plunging ranula that appeared septate on ultrasound and CT scans was previously described by O'Connor and McGurk.2 Although the histology confirmed the lesion to be a ranula, there was never any mention of it being a multicystic lesion. This concurs with the lesion described here which appeared multilocular on MRI but could not be assessed as such histologically due to the large size of the locules.
An explanation for this particular radiological presentation might be that the mucin, on tracking through the tissues, caused a separation of loose connective tissue in various planes resulting in multiple locules. Thus a plunging ranula may present radiologically either as a unilocular or a multi-locular lesion.
Other conditions which may be considered in a differential diagnosis include salivary duct cysts, dermoid cysts, thyroglossal cysts, branchial cysts and cystic hygromas. Dermoid cysts are usually confined to the midline while cystic hygromas, a variety of lymphangioma, exhibit large cavernous spaces in the floor of the mouth. Salivary duct cysts are mucous retention cysts, and as true cysts are epithelial lined. This feature will be evident on histology. Thyroglossal and branchial cysts are developmental cysts which arise from embryonic elements that persist post-natally. Thyroglossal cysts commonly show a midline swelling in the neck below the hyoid bone and are more prevalent within the first two years of life while branchial cysts present laterally in the neck along the anterior border of the sternomastoid muscle.1
Various treatment modalities for treatment of ranulas have been reported in the literature. Simple ranulas are often treated by marsupialisation. This involves removal of the roof of the intraoral lesion allowing the sublingual ducts to communicate with the oral cavity.1 Marsupialisation and packing of the cyst has also been advocated but removal of the sublingual gland with drainage only, with partial or complete removal of the cyst are more successful options for the treatment of plunging ranulas.1,3 These surgical modalities are often associated with known complications such as infection, bleeding, haematoma formation and paraesthesia of the tongue. Injury to the submandibular duct and recurrence are common complications.4
Marsupialisation produces the highest recurrence rate while removal of the sublingual gland together with partial or complete removal of the cyst carries the lowest recurrence rate1,3,4
Since the lesion described presented with a multilocular appearance on MRI, a more extensive surgical approach seemed necessary. Consequently removal of the sublingual gland and complete excision of the multilocular lesion was chosen as the procedure of choice, with the objectives of not only removing the pathology but also preventing recurrence. Hence the sublingual gland was removed via an intraoral approach while the multilocular cyst was dissected by means of a submandibular approach in order to ensure its complete removal.
Conflict of Interest: None declared
References
1. Neville BD, Damm DD, Allen CM, Bouquot JE. Oral and Maxillo-facial Pathology. 2nd ed. Philadelphia: Saunders, 2002: 391-2. [ Links ]
2. O'Connor R, Mc-Gurk M. The plunging ranula: diagnostic difficulties and a less invasive approach to treatment. Int J of Oral and Maxillofacial Surgery 2013; 42: 1469-74. [ Links ]
3. Yunsu Y, Kihwan J. Surgical results of the intraoral approach for plunging ranula. Acta Oto-Laryngologica 2014; 134: 201-5. [ Links ]
4. Chidzonga MM, Mahova L. Ranula: Experience with 83 cases in Zimbabwe. J Oral Maxillofac Surg 2007; 65: 79-82. [ Links ]
 Correspondence:
Correspondence:
B Buch
Department of General Dental Practice
School of Oral Health Sciences
University of the Witwatersrand
Johannesburg
Tel: 011 488 4854
Email: Brian.Buch@wits.ac.za













