Serviços Personalizados
Artigo
Indicadores
Links relacionados
-
 Citado por Google
Citado por Google -
 Similares em Google
Similares em Google
Compartilhar
South African Dental Journal
versão On-line ISSN 0375-1562
versão impressa ISSN 0011-8516
S. Afr. dent. j. vol.69 no.8 Johannesburg 2014
CASE BOOK
Oral medicine case book 63: HIV-associated oral melanin hyperpigmentation
R ChandranI; RAG KhammissaII; J LemmerIII; L FellerIV
IBDS MSc (Dent) DPH MSc (Dent) OP Department of Periodontology and Oral Medicine, University of Limpopo, Medunsa Campus, South Africa
IIBChD PDD MSc(Dent) MDent (OMP). Department of Periodontology and Oral Medicine, University of Limpopo, Medunsa Campus, South Africa
IIIBDS HDipDent FCD (SA) OMP FCMSAae Hon. FCMSA. Department of Periodontology and Oral Medicine, University of Limpopo, Medunsa Campus, South Africa
IVDMD MDent (OMP). Department of Periodontology and Oral Medicine, University of Limpopo, Medunsa Campus, South Africa
ACRONYMS
aMSH: alpha melanocyte stimulating hormone
HAART: highly active antiretroviral therapy
MC1R: melanocortin 1 receptor
OMH: Oral melanin hyperpigmentation
HIV-OMH: HIV associated oral melanin hyperpigmentation
INTRODUCTION
Oral melanin hyperpigmentation (OMH) is not uncommon in HIV+ persons1 In Venezuela (38%)5 and in India (30%)3 HIV-associated OMH (HIV-OMH) is quite common, but by contrast is substantially less common in Italy (6.4%)4 and in sub-Saharan Africa (Tanzania, 4.7%, Kenya, 6%).5,6 In South Africa, the national prevalence of HIV-OMH is unknown, but Arendorf et al., 1998, reported a prevalence of less than 1% in the population of greater Cape Town, although the authors could not differentiate with confidence between coloured and black South Africans, and they had not been able to exclude other causes for the melanin hyperpigmentation.6
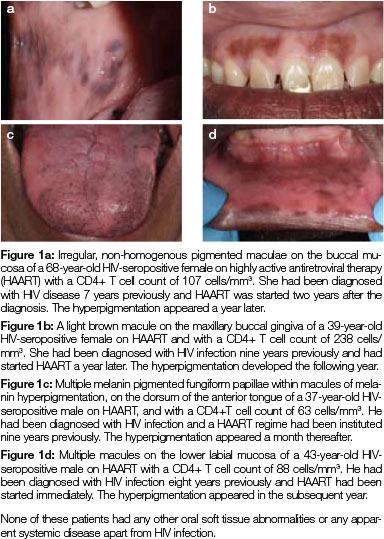
HIV-OMH (Figure 1) may develop secondarily to HIV-induced upregulation of pro-inflammatory cytokines, to drugs used in treating HIV disease or concomitant associated diseases (zidovudine, clofazimine and ketoconazole), or to adrenocortical insufficiency, which frequently occurs in HIV+ persons with low CD4+ T cell counts. HIV-OMH may also be idiopathic. The increased melanin in HIV-OMH is located either in the epithelial basal cell layer, in melanophages in the lamina propria or at both sites.1,8-10
Both brown-black eumelanin and yellow-red pheomelanin are synthesized in melanosomes which are membrane-bound organelles within melanocytes. These melanosomes contain all the proteins and enzymes necessary for melanogenesis. Mela-nogenesis is a complex process controlled locally by multiple factors including alpha melanocyte stimulating hormone (aMSH) produced by keratinocytes and melanocytes, melanocytic melanocortin-1 receptors (MC1R), adrenergic and cholinergic agents, and cytokines in the microenvironment. The type and the amount of melanin produced is genetically determined11
Oral mucosal and epidermal melanocytes are histologically and ultrastructurally identical, but it is recognised that oral melanocytes under physiological conditions are inherently less active metabolically13 Nevertheless, when stimulated by hormones, pro-inflammatory cytokines, tobacco smoke or infectious agents such as HIV, oral mucosal melanocytes may become active, producing melanin hyperpigmentation12,13
DISCUSSION
Melanocytes originate from precursor cells which during development migrate from the neural crest, and ultimately differentiate into mature melanocytes that reside in the basal and suprabasal layers of the epidermis, and of the epithelium of mucous membranes14 Apart from their primary role in melanogenesis, melanocytes function as immune cells producing cytokines which modulate local immuno-inflam-matory and antibacterial responses, and as neuroendocrine cells producing acetylcholine, catecholamines, opioids and melanocortins, all of which contribute to tissue homeostasis11 Melanin plays an essential role in protection against ultraviolet radiation, and also provides protection against other environmental stressors such as reactive oxygen species, and is a main determinant of the colour of skin, hair and eyes12,15
Melanocytes and their neighbouring keratinocytes form epithelial melanin units, each unit consisting of one melanocyte and a group of up to 36 keratinocytes16 The melanin-containing melanosomes produced by the melanocytes are transferred via the dendritic processes of the melanocytes to the keratinocytes within the unit16 Skin and oral mucosa owe their colour to the number and size of melanosomes, whether these contain eumelanin or pheomelanin, to the state of maturation of the network of melanocytic dendritic processes, and to the efficacy with which these dendritic processes distribute the melanosomes to neighbouring keratinocytes.17,18
Melanin biosynthesis is genetically determined and there are substantial differences in the degree of melanin pigmentation among racial/ethnic groups and between subjects of the same group. Both oral mucosal physiological/racial melanin hyperpigmentation19 and HIV-OMH are more frequently seen in darker than in lighter skinned subjects.20
If it occurs, HIV-OMH usually appears within two years of the diagnosis of HIV infection, or after a month or more of antiretroviral medication with zidovudine,21 and it is observed more frequently in HIV+ persons with a CD4+ T cell count of less than 200 cells/cubic mm.22 It appears that HIV-OMH is brought about by upregulation of activation of normal oral melanocytes by HIV infection or by zidovudine with consequent increased production of melanin.4 As it is ethically unjustifiable to biopsy HIV-OMH, it is not clear what role is played by an increase in the number of melanocytes, by an increase in the number of melanosomes, or by a shift in the type of melanin produced, in the pathogenesis of HIV-OMH.
It has been proposed that IL-1, IL-6 and TNF-α, which are upregulated during HIV infection, stimulate keratinocytes and melanocytes to produce a MSH, and stimulate melanocytes to express MC1R, thus resulting in increased melanogenesis by melanocytes, triggering the formation of HIV-OMH.9 The fact that HIV-induced cytokine upregulation in HIV+ persons is inversely proportional to their CD4+ T cell counts may explain the observation that HIV-OMH occurs most frequently in HIV+ persons with low CD4+T cell counts.22 HIV-OMH manifests clinically as single or as multiple brownish or brown-black macules or as ill-defined diffuse areas of melanin hyperpigmentation (Figure 1).
This hyperpigmentation may affect any part of the oral mucosa, but most frequently the buccal mucosa.23 Although HIV-OMH does not have any clinical or pathological significance, it needs to be differentiated from similar pathologically hyperpigmented oral mucosal lesions or conditions including Addison's disease, Albright's syndrome, neurofibromatosis, smoker's melanosis, atypical melanocytic proliferations and melanomas.23,24 These can usually be distinguished on the basis of a good medical history: but if hyperpigmentation follows a diagnosis of HIV infection or follows the initiation of HIV-related medication, then a diagnosis of HIV-OMH should be considered.25
Further research is needed in order to discover what mechanisms and environmental factors possibly play a role in the pathogenesis of HIV-OMH and whether HIV-OMH has any clinical significance in HIV disease.25
References
1. Scully C, Laskaris G, Pindborg J, Porter SR, Reichart P Oral manifestations of HIV infection and their management. II. Less common lesions. Oral Surg Oral Med Oral Pathol 1991;71:167-71. [ Links ]
2. Bravo IM, Correnti M, Escalona L, Perrone M, Brito A, Tovar V, et aJ. Prevalence of oral lesions in HIV patients related to CD4 cell count and viral load in a Venezuelan population. Med Oral Patol Oral Cir Bucal 2006;11:E33-9. [ Links ]
3. Sontakke SA, Umarji HR, Karjodkar F Comparison of oral manifestations with CD4 count in HIV-infected patients. Indian J Dent Res 2011 ;22:732, DOI: 10.4.4103/0970-9290.93470. [ Links ]
4. Ficarra G, Shillitoe EJ, Adler-Storthz K, Gaglioti D, Di Pietro M, Riccardi R, et aJ. Oral melanotic macules in patients infected with human immunodeficiency virus. Oral Surg Oral Med Oral Pathol 1990;70:748-55. [ Links ]
5. Hamza OJ, Matee MI, Simon EN, Kikwilu E, Moshi MJ, Mugusi F, et a. Oral manifestations of HIV infection in children and adults receiving highly active anti-retroviral therapy [HAART] in Dar es Salaam, Tanzania. BMC Oral Health 2006;6:12. [ Links ]
6. Butt FM, Chindia ML, Vaghela VP Mandalia K. Oral manifestations of HIV/AIDS in a Kenyan provincial hospital. East Afr Med J 2001;78:398-401. [ Links ]
7. Arendorf TM, Bredekamp B, Cloete CA, Sauer G. Oral manifestations of HIV infection in 600 South African patients. J Oral Pathol Med 1998;27:176-9. [ Links ]
8. Zhang X, Langford A, Gelderblom H, Reichart P Ultrastructural findings in oral hyperpigmentation of HIV-infected patients. J Oral Pathol Med 1989;18:471-4. [ Links ]
9. Smith KJ, Skelton HG, Heimer W, Baxter D, Angritt P Frisman D, et aJ. Melanocytic activation in HIV-1 disease: HMB-45 staining in common acquired nevi. Military Medical Consortium for the Advancement of Retroviral Research. J Am Acad Dermatol 1993;29:539-44. [ Links ]
10. Porter SR, Glover S, Scully C. Oral hyperpigmentation and adrenocortical hypofunction in a patient with acquired immunodeficiency syndrome. Oral Surg Oral Med Oral Pathol 1990;70:59-60. [ Links ]
11. Slominski A, Tobin DJ, Shibahara S, Wortsman J. Melanin pigmentation in mammalian skin and its hormonal regulation. Physiol Rev 2004;84:1155-228. [ Links ]
12. Feller L, Masilana A, Khammissa RA, Altini M, Jadwat Y Lemmer J. Melanin: the biophysiology of oral melanocytes and physiological oral pigmentation. Head Face Med 2014;10:8.DOI: 10.1186/1746-160x-10-8. [ Links ]
13.Barrett AW, Scully C. Human oral mucosal melanocytes: a review, J Oral Pathol Med 1994;23:97-103. [ Links ]
14.Thomas AJ, Erickson CA. The making of a melanocyte: the specification of melanoblasts from the neural crest. Pigment Cell Melanoma Res 2008;21:598-610. [ Links ]
15.Plonka PM, Grabacka M. Melanin synthesis in microorgan-isms--biotechnological and medical aspects. Acta Biochim Pol 2006;53:429-43. [ Links ]
16.Nordlund JJ. The melanocyte and the epidermal melanin unit: an expanded concept. Dermatol Clin 2007;25:271-81. [ Links ]
17. Sturm RA. Molecular genetics of human pigmentation diversity. Hum Mol Genet 2009;18:R9-17. [ Links ]
18. Lin JY Fisher DE. Melanocyte biology and skin pigmentation. Nature 2007;445:843-50. [ Links ]
19. Amir E, Gorsky M, Buchner A, Sarnat H, Gat H. Physiologic pigmentation of the oral mucosa in Israeli children. Oral Surg Oral Med Oral Pathol 1991;71:396-8. [ Links ]
20. Eversole RE. Pigmented Lesions of the Oral Mucosa. In: Greenberg MS, Glick M, editors. Burket's Oral Medicine Diagnosis and Treatment. 10 ed. Hamilton, Ontario: BC Decker Inc; 2003; 126-36. [ Links ]
21. Greenberg RG, Berger TG. Nail and mucocutaneous hyperpigmentation with azidothymidine therapy. J Am Acad Dermatol 1990;22:327-30. [ Links ]
22. Blignaut E, Patton LL, Nittayananta W, Ramirez-Amador V, Ran-ganathan K, Chattopadhyay A. (A3) HIV Phenotypes, oral lesions, and management of HIV-related disease. Adv Dent Res 2006;19:122-9. [ Links ]
23. Langford A, Pohle HD, Gelderblom H, Zhang X, Reichart PA. Oral hyperpigmentation in HIV-infected patients. Oral Surg Oral Med Oral Pathol 1989;67:301-7, [ Links ]
24. Alawi F, Pigmented lesions of the oral cavity: an update. Dent Clin North Am 2013;57:699-710. [ Links ]
25.Feller L, Chandran R, Kramer B, Khammissa RAG, Altini M, Lemmer J. Melanocyte biology and function with reference to oral melanin hyperpigmentation in HIV-seropositive subjects. AIDS Res Hum Retroviruses 2014; 30:837-43. [ Links ]
 Correspondence:
Correspondence:
L Feller
Head: Dept. Periodontology and Oral Medicine
Box D26 School of
Dentistry, MEDUNSA 0204
South Africa.
Tel: (012) 521 4834
E-mail: liviu.feller@ul.ac.za













